Hematological alterations in the large burned patient
Abstract
Introduction: The serious burns alter of significant way the hematological and coagulation parameters.
Objective: To describe the hematological alterations in the large burned patient.
Methods: A descriptive, longitudinal and prospective study was carried out for the sake of describing the main hematological alterations in the large burned patient, once 2020 were deposited in the Manuel Ascunce Domenech's Universitary Hospital service of Plastic Surgery and Caumatology, of the City Camagüey, during the period understood between May, 2020 to April, 2022. They studied 38 patients in those who they had in account variables: hematological alteration, corporal burned-out surface, index forecast, state to the discharge.
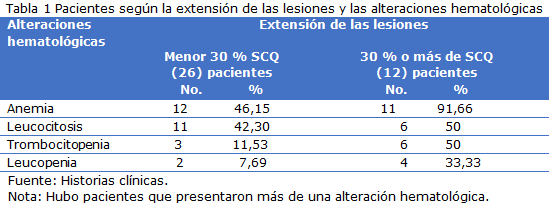
Results: Of the patients with 30 % or more of corporal burned-out surface (12 in total) the 91.66 % presented anemia. Anemia was found with more frequency in the patient classified as very serious condition, 11 patients that represent the 28.95 %, it is from standing out that the patients with this severity rate constituted the majority in this series, 19 for a 50 %. In 23 of the sick persons of this series they presented leukocytal alterations. Leucocytosis was found in 44.73 % of the patients, and leukopenia in six patients which represented 15.79 %. In 23.68 % of the patients the presence of thrombocytopenia was observed.
Conclusions: Hematological alterations influence the good progress of burned patients, and if not treated in a timely manner can lead to death.
DeCS: BURNS/complications; HEMATOLOGY; THROMBOCYTOPENIA; ANEMIA; PROGNOSIS.
Downloads
References
1. Abdilkarim DA. Medical Investigation and Clinical Changes in the Early Phases of Post Burn Adult Inpatients as Indicators for Prompt Infection Diagnosis, in the Hospital for Burn and Plastic Surgery, Sulaimanyah, Iraq. Iraqi National Journal of Medicine [Internet]. 2022 [citado 25 Abr 2023];4(1):1-14. Disponible en: https://www.iasj.net/iasj/download/bb43eef73c2767e5
2. Organización Mundial de la Salud [Internet]. Ginebra: OMS; 2018 [actualizado 2024; citado 01 Oct 2023]. Quemaduras;[aprox. 2p.] Disponible en: https://www.who.int/es/news-room/fact-sheets/detail/burns
3. Burgess M, Valdera F, Varon D, Kankuri E, Nuutila K. The Immune and Regenerative Response to Burn Injury. Cells [Internet]. 2022 [citado 25 Abr 2023];11(19):3073. Disponible en: https://www.mdpi.com/2073-4409/11/19/3073
4. de la Cruz García G. Utilidad de la eritropoyetina en el paciente quemado grave con anemia. Revisión del tema. Gac Méd Espirit [Internet]. 2020 [citado 25 Feb 2023];22(1):60-70. Disponible en: http://scielo.sld.cu/pdf/gme/v22n1/1608-8921-gme-22-01-60.pdf
5. Puentes Marrugo AD, Salgar Sarmiento DA. Disminución posoperatoria de hemoglobina en paciente quemado, dependiente de procedimiento quirúrgico, superficie y grado de quemadura [tesis]. Bogotá: Universidad el Bosque; 2019 [citado 23 Feb 2024]. Disponible en: https://docplayer.es/210442955-Disminucion-posoperatoria-de-hemoglobina-en-paciente-quemado-dependiente-de-procedimiento-quirurgico-superficie-y-grado-de-quemadura.html
6. Moya Rosa EJ, Moya Corrales Y. Complicaciones en los pacientes quemados. Arch méd Camagüey [Internet]. 2022 [citado 25 Feb 2023];26:e9306. Disponible en: https://revistaamc.sld.cu/index.php/amc/article/download/9306/4495
7. Giraldo Salazar OL, Hoyos Franco M, Negrete Álvarez C. Morbilidad perioperatoria de pacientes con quemaduras mayores del 5 % de la superficie corporal total en el Hospital Universitario San Vicente Fundación-Medellín [tesis]. Colombia: Universidad de Antioquia; 2020 [citado 05 Oct 2023]. Disponible en: https://www.redalyc.org/journal/120/12068044008/html/
8. Sen S, Hsei L, Tran N, Romanowski K, Palmieri T, Greenhalgh D, et al. Early clinical complete blood count changes in severe burn injuries. Burns [Internet]. 2019 [citado 5 Oct 2023];45(1):97-10. Disponible en: https://www.sciencedirect.com/science/article/abs/pii/S0305417918305874?via%3Dihub
9. Betar N, Warren J, Adams J, Herbert D, Vujcich E, Maitz P, et al. Iron status in patients with burn anaemia. Burns [Internet]. 2022 [citado 25 Feb 2023];49(3):701-706. Disponible en: https://pubmed.ncbi.nlm.nih.gov/35715343/
10. Tichil I, Rosenblum S, Paul E , Cleland H. Treatment of Anaemia in Patients with Acute Burn Injury: A Study of Blood Transfusion Practices. J Clin Med [Internet]. 2021 [citado 25 Feb 2023];10(3):476. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7865424/
11. Koljonen V, Tuimala J, Haglund C, Tukiainen E, Vuola J, Juvonen E, et al. The Use of Blood Products in Adult Patients with Burns. Scandinavian Journal of Surgery [Internet]. 2016[citado 25 Feb 2023];105(3):178-185. Disponible en: https://journals.sagepub.com/doi/epub/10.1177/1457496915622127
12. Walczak J, Bunn C, Saini P, Liu YM, Baldea AJ, Muthumalaiappan K. Transient Improvement in Erythropoiesis Is Achieved Via the Chaperone AHSP With Early Administration of Propranolol in Burn Patients. J Burn Care Res [Internet]. 2021 [citado 25 Feb 2023];42(2):311-322. Disponible en:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7940505/
13. Spiridonova TG, Zhirkova E. Etiology and Pathogenesis of Burn Anemia. The Role of the Blood Transfusion in the Treatment of Patients with Burns. Journal Emergency Medical Care [Internet]. 2018 [citado 25 Feb 2023];7(3):244-252. Disponible en: https://www.jnmp.ru/jour/article/view/506/576
14. Koljonen V, Tuimala J, Haglund C, Tukiainen E, Vuola J, Juvonen E, et al. The Use of Blood Products in Adult Patients with Burns. Scand J Surg [Internet]. 2016 [citado 25 Feb 2023];105(3):178-185. Disponible en: https://pubmed.ncbi.nlm.nih.gov/26929291/
15. Osuka A, Ishihara T, Shimizu K, Shintani A, Ogura H, Ueyama M. Natural kinetics of blood cells following major burn: Impact of early decreases in white blood cells and platelets as prognostic markers of mortality. Burns [Internet]. 2019 [citado 25 Feb 2023];45(8):1901-1907. Disponible en:
https://sci-hub.se/downloads/2019-11-10/94/osuka2019.pdf
16. Koval MG, Sorokina EY, Tatsiuk SV, Badiuk NS. Peculiarities of the severe burn disease course leading to sepsis and mod in children. Pharmacology Online [Internet]. 2021[citado 25 Feb 2023];1:20-29. Disponible en: https://pharmacologyonline.silae.it/files/archives/2021/vol1/PhOL_2021_1_A004_Koval.pdf
17. Jeschke MG, van Baar ME, Choudhry MA, Chung KK, Gibran NS, Logsetty S. Burn injury. NATURE REVIEWS [Internet]. 2020 [citado 25 May 2023];6(11):1-25.
Disponible en: https://www.nature.com/articles/s41572-020-0145-5.pdf?pdf=button%20sticky
18. Hernández-Patiño I, Blas-Mas S, Burgos J, De La Crus-Vargas J. Factores asociados a infección intrahospitalaria en adulto gran quemado en hospital de referencia peruano. Estudio de 5 años. Cir. plást. Iberolatinoam [Internet]. 2022 [citado 25 May 2023];48(3):[aprox. 12 p]. Disponible en: https://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0376-78922022000300012
19. Żwierełło W, Piorun K, Skórka-Majewicz M, Maruszewska A, Antoniewski J, Gutowska I. Burns: Classification, Pathophysiology, and Treatment: A Review. Int J Mol Sci [Internet]. 2023 [citado 25 May 2023];24(4):3749. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9959609/
20. Mulder PPG , Koenen HJPM, Vlig M, Joosten I, de Vries RBM, Boekema VKHL. Burn-Induced Local and Systemic Immune Response: Systematic Review and Meta-Analysis of Animal Studies. J Invest Dermatol [Internet]. 2022 [citado 25 May 2023]; 142(11):3093-3109. Disponible en: https://pubmed.ncbi.nlm.nih.gov/35623415/
21. Barbier JM, Viana MV, Pantet O, Alberio L, Berger MM. Blood coagulation alterations over the first 10 days after severe burn injury. Burns Open [Internet]. 2022 [citado 25 May 2023];6(1):10-18. Disponible en: https://www.sciencedirect.com/science/article/pii/S246891222100105X
22. Güldoğan CE, Kendirci M, Gündoğdu E, Yastı A. Analysis of factors associated with mortality in major burn patients. Turk J Surg [Internet]. 2019 [citado 25 Mar 2023];35(3):155-164. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6795231/
23. Alehi H, Moienian E, Rahbar A, Salehi SAH, Momeni M. Prevalence of thrombocytopenia in the first week after burn injury and its relation ship with burn severity in Shahid Motahari Hospital over a period of 6 months in 2017. Annals of Burns and Fire Disasters [Internet]. 2022 [citado 25 May 2023];61(1):1-11. Disponible en:
http://www.medbc.com/meditline/articles/vol_61/num_1/text/vol61n1p1474.pdf
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Keiler Patiño-Gómez, Enrique Joaquín Moya-Rosa, Gustavo Tapia-Mesa

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright: Camagüey Medical Archive Magazine, offers immediately after being indexed in the SciELO Project; Open access to the full text of the articles under the principle of making available and free the research to promote the exchange of global knowledge and contribute to a greater extension, publication, evaluation and extensive use of the articles that can be used without purpose As long as reference is made to the primary source.
Conflicts of interest: authors must declare in a mandatory manner the presence or not of conflicts of interest in relation to the investigation presented.
(Download Statement of potential conflicts of interest)
The Revista Archivo Médico de Camagüey is under a License Creative Commons Attribution-Noncommercial-No Derivative Works 4.0 International (CC BY 4.0).
This license allows others to distribute, to mix, to adjust and to build from its work, even for commercial purposes, as long as it is recognized the authorship of the original creation. This is the most helpful license offered. Recommended for maximum dissemination and use of licensed materials. The full license can be found at: https://creativecommons.org/licenses/












 22 julio 2025
22 julio 2025