Risk factors associated with clinical worsening of patients admitted with Alzheimer's disease
Abstract
Introduction: The main cause of degenerative dementia is Alzheimer's disease. In the Cuban population, one in four people aged 65 and over dies from this disease or another form of dementia.
Objective: To identify the risk factors associated with the clinical worsening of patients admitted with Alzheimer's disease at the Rene Vallejo Ortiz University Psychiatric Hospital.
Methods: An observational, descriptive and cross-sectional study was carried out. The universe was made up of all patients admitted to the aforementioned healthcare and teaching institution. The non-probabilistic sample and at the discretion of the authors was made up of 77 adult patients with the diagnosis of the disease in the indicated study period between January 2013 and December 2022. Medical records were the secondary source of information. Descriptive and inferential statistics were used. The information was summarized in tables and graphics.
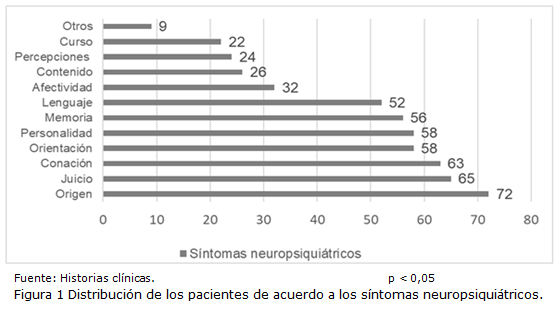
Results: 90.6% were over 60 years old and more than half were male (54.5%). Most patients presented various associated symptoms. Personality and orientation disorders were found in 75.3%, while memory disorders were found in 72.7%.
Conclusions: The clinical worsening after hospital admission was accentuated in those patients without schooling, single, unemployed, with cerebrovascular diseases and presence of dysfunctional families. Anemic patients or patients with signs of focal cortical irritation in the frontoparietal region with secondary generalization mostly presented clinical worsening.
DeCS: ALZHEIMER DISEASE; INPATIENTS; RISK FACTORS; DEMENTIA; SIGNS AND SYMPTOMS.
Downloads
References
1. Khan TK. An Algorithm for Preclinical Diagnosis of Alzheimer’s Disease. Front Neurosci [Internet]. 2018 [citado 15 Ago 2023];12:275. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5936981/pdf/fnins-12-00275.pdf
2. Pérez Rodríguez M, Álvarez Gómez T, Martínez Badaló EJ, Valdivia Cañizares S, Borroto Carpio I, Pedraza Núñez H. El síndrome del cuidador en cuidadores principales de ancianos con demencia Alzhéimer. Gac Méd Espirit [Internet] 2017 [citado 15 Ago 2023];19(1). Disponible en: https://revgmespirituana.sld.cu/index.php/gme/article/view/517/html
3. Tellechea P, Pujol N, Esteve-Belloch P, Echeveste B, García-Eulate MR, Arbizu J, et al. Early- and late-onset Alzheimer disease: Are they the same entity? Neurología [Internet]. 2018 [citado 15 Ago 2023];33(4):244-55. Disponible en: https://doaj.org/article/1d14674b8463488b82daef2893e4d4fa
4. Aranda M, Calabria A. Impacto económico-social de la enfermedad de Alzheimer. Neurol Arg [Internet]. 2019 Ene-Mar [citado 15 Ago 2023];11(1):19-26. Disponible en: https://www.elsevier.es/es-revista-neurologia-argentina-301-articulo-impacto-economico-social-enfermedad-alzheimer-S1853002818300831
5. Balea Fernández FJ, Alonso Ramírez J. Biomarcadores en la demencia tipo Alzheimer: sistema sanitario y edadismo. International Journal of Developmental and Educational Psychology [Internet]. 2020 [citado 15 Ago 2023];1(1):247-54. Disponible en: https://www.redalyc.org/journal/3498/349863388025/html/
6. Cubinkova V, Valachova B, Uhrinova I, Brezovakova V, Smolek T, Jadhav S, et al. Alternative hypotheses related to Alzheimer’s disease. Bratisl Lek Listy [Internet]. 2018 [citado 15 Ago 2023];119(4):210-16. Disponible en: http://www.elis.sk/download_file.php?product_id=5631&session_id=h7ntgagt03pvbn10a94l80h5k7
7. Romero-Vanegas SJ, Vargas-González JC, Pardo R, Eslava-Schmalbach J, Moreno- Angarita M. El sistema de salud colombiano y el reconocimiento de la enfermedad de Alzheimer. Rev Salud Pública [Internet]. 2021 [citado 15 Ago 2023];23(2):1-9. Disponible en: https://revistas.unal.edu.co/index.php/revsaludpublica/article/view/88369/82248
8. Nebel RA, Aggarwalb NT, Barnes LL, Gallaghera A, Goldsteinc JM, Kantarcie K, et al. Understanding the impact of sex and gender in Alzheimer's disease: A call to action. Alzheimers Dement [Internet]. 2018 Sep [citado 21 Ago 2023];14(9):1171-83. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6400070/
9. Espín Falcón JC. Factores de riesgo asociados a pacientes con enfermedad de Alzheimer y sus cuidadores principales. Rev cuban med gen integr [Internet]. 2020 [citado 15 Ago 2023];36(1). Disponible en: https://revmgi.sld.cu/index.php/mgi/article/view/1138
10.Prince M, Ali GC, Guerchet M, Prina AM, Albanese E, Wu YT. Recent global trends in the prevalence and incidence of dementia, and survival with dementia. Alzheimer’s Res Ther [Internet]. 2016 [citado 21 Ago 2023];8:23. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4967299/
11. Fiest KM, Roberts JI, Maxwell CJ, Hogan DB, Smith EE, Frolkis A, et al. The Prevalence and Incidence of Dementia Due to Alzheimer’s Disease: a Systematic Review and Meta-Analysis. Can J Neurol Sci [Internet] 2016 Abr [citado 21 Ago 2023];43(Suppl 1):S51-82. Disponible en: https://www.cambridge.org/core/journals/canadian-journal-of-neurological-sciences/article/prevalence-and-incidence-of-dementia-due-to-alzheimers-disease-a-systematic-review-and-metaanalysis/5456A8F9818DAE7764EFC942ADCF0A98
12. Seshadri S, Wolf PA, Beiser A, Au R, McNulty K, White R, et al. Lifetime risk of dementia and Alzheimer’s disease. The impact of mortality on risk estimates in the Framingham Study. Neurology [Internet]. 1997 Dic [citado 21 Ago 2023];49(6):1498-504. Disponible en: https://n.neurology.org/content/49/6/1498
13. Podcasy JL, Neill Epperson N. Considering sex and gender in Alzheimer disease and other dementias. Dialogues Clin Neurosci [Internet]. 2016 Dic [citado 21 Ago 2023];18(4):437-46. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5286729/
14. Pike CJ. Sex and the development of Alzheimer’s disease. J Neurosci Res [Internet]. 2017 Ene [citado 21 Ago 2023];95(1-2):671-80. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5120614/
15. Hakansson K, Rovio S, Helkala EL, Vilska AR, Winblad B, Soininen H, et al. Association between mid-life marital status and cognitive function in later life: population based cohort study. BMJ [Internet]. 2009 [citado 21 Ago 2023];339: b2462. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2714683/
16. Fan LY, Sun Y, Lee HJ, Yang SC, Chen TF, Lin KN, et al. Marital status, lifestyle and dementia: a Nationwide survey in Taiwan. PLoS One [Internet]. 2015 [citado 21 Ago 2023];10(9):e0139154. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4587383/
17. Sommerlad A, Ruegger J, Singh-Manoux A, Lewis G, Livingston G. Marriage and risk of dementia: systematic review and meta-analysis of observational studies. J Neurol Neurosurg Psychiatry [Internet]. 2018 Mar [citado 21 Ago 2023];89(3):231-8. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5869449/
18. Kobayashi E, Nakano M, Kubota K, Himuro N, Mizoguchi S, Chikenji T, et al. Activated forms of astrocytes with higher GLT-1 expression are associated with cognitive normal subjects with Alzheimer pathology in human brain. Sci Rep [Internet]. 2018 Ene [citado 21 Ago 2023];8(1):1712. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5786045/
19. Serrano-Pozoa A, Growdon JH. Is Alzheimer’s Disease Risk Modifiable? J Alzheimers Dis [Internet]. 2019 [citado 21 Ago 2023];67(3):795-819. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6708279/
20. Chhatwal JP, Schultz AP, Johnson KA, Hedden T, Jaimes S, Benzinger TLS, et al. Preferential degradation of cognitive networks differentiates Alzheimer’s disease from ageing. Brain [Internet]. 2018 May [citado 21 Ago 2023];141(5):1486-500. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5917745/
21. Lu FP, Lin KP, Kuo HK. Diabetes and the risk of multi-system aging phenotypes: a systematic review and meta-analysis. PLoS One [Internet]. 2009 [citado 15 Ago 2023]; 4(1): e4144. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2607544/
22. He W, Ruan Y, Yuan C, Luan X , He J. Hemoglobin, anemia, and poststroke cognitive impairment: A cohort study. Int J Geriatr Psychiatry [Internet]. 2020 May [citado 15 Ago 2023];35(5):564-71. Disponible en: https://onlinelibrary.wiley.com/doi/10.1002/gps.5272
23. Wolters FJ, Zonneveld HI, Licher S, Cremers LGM, Kamran Ikram M, Koudstaal PJ, et al. Hemoglobin and anemia in relation to dementia risk and accompanying changes on brain MRI. Neurology [Internet]. 2019 Ago [citado 15 Ago 2023];93(9):e917-e926. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6745727/
24. Bhat S, Acharya R, Dadmehr N, Adeli H. Clinical Neurophysiological and Automated EEG-Based Diagnosis of the Alzheimer’s Disease. Eur Neurol [Internet]. 2015 [citado 21 Ago 2023];74(3-4):202-10. Disponible en: https://karger.com/ene/article/74/3-4/202/125227/Clinical-Neurophysiological-and-Automated-EEG
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Wilson Antonio Pérez-Nicolaes, Ignacio Cabrera-Figueredo, Kelvis Dayron Castillo-Esquivel, María Georgina Nicolaes-Hernández, Grethel Camejo-Sampedro

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright: Camagüey Medical Archive Magazine, offers immediately after being indexed in the SciELO Project; Open access to the full text of the articles under the principle of making available and free the research to promote the exchange of global knowledge and contribute to a greater extension, publication, evaluation and extensive use of the articles that can be used without purpose As long as reference is made to the primary source.
Conflicts of interest: authors must declare in a mandatory manner the presence or not of conflicts of interest in relation to the investigation presented.
(Download Statement of potential conflicts of interest)
The Revista Archivo Médico de Camagüey is under a License Creative Commons Attribution-Noncommercial-No Derivative Works 4.0 International (CC BY 4.0).
This license allows others to distribute, to mix, to adjust and to build from its work, even for commercial purposes, as long as it is recognized the authorship of the original creation. This is the most helpful license offered. Recommended for maximum dissemination and use of licensed materials. The full license can be found at: https://creativecommons.org/licenses/












 22 julio 2025
22 julio 2025