Neurocutaneous melanosis: a case report
Abstract
Background: neurocutaneous melanosis is a non-hereditary congenital disorder characterized by the association of multiple or large pigmented nevus and an excessive proliferation of melanocytes in the central nervous system. Neurological symptoms are usually of early onset in the infant stage with convulsions of difficult control, making the forecast reserved.
Objective: to present a case with clinical diagnosis of neurocutaneous melanosis with neurological manifestations such as seizures from the infant stage.
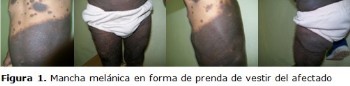
Clinical case: a male patient born with a giant melanoma stain that extends from the thorax to the abdomen, inguinal region, genital and lower limbs as a dressing. In the posterior region of the back, it begins in both flanks, sacral region until the misty of both legs, presenting convulsions at one month old. Continuing the appearance of hyperpigmented spots all over the body, which at the age of life are larger darker accompanied by thick hair, with epileptic seizures refractory to treatment.
Conclusions: this disease that is produced by the increase of melanin to the skin and the central nervous system requires a monitoring of dermal lesions and a control of seizures, considering the importance of neurodevelopmental follow-up in a multidisciplinary way for timely intervention if necessary.
DeCS: NEVUS, PIGMENTED; NEVI AND MELANOMAS; CONGENITAL ABNORMALITIES; CHILD, PRESCHOOL; CASE REPORTS.
Downloads
References
1.Criscito MC, Correa LM, Koshenkov VP, Firoz BF. Recurrent Nevi in a Skin Graft Following Excision of Giant Congenital Melanocytic Nevus. Dermatol Surg [Internet]. 2016 Sep [citado 2017 Jan 20];42(9):[about 9 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27227469
2.Chokoeva AA, Fioranelli M, Roccia MG, Lotti T, Wollina U, Tchernev G. Giant congenital melanocytic nevus in a bulgarian newborn. J Biol Regul Homeost Agents [Internet]. 2016 Apr-Jun [citado 2017 Jan 20];30:[about 9 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27373137
3.Ding JP, Chen B, Fang L, Wang LZ. Total reconstruction of giant congenital circumferential nevi of the upper limb using a large pedicle expanded flank flap: A brief report. Ann R Coll Surg Engl [Internet]. 2016 Nov [citado 2017 Jan 20];98(8):[about 2 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27652668
4.Lalor L, Busam K, Shah K. Prepubertal Melanoma Arising within a Medium-Sized Congenital Melanocytic Nevus. Pediatr Dermatol [Internet]. 2016 Nov [citado 2017 Jan 20];33(6):[about 9 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27573553
5.Bekiesinska-Figatowska M, Sawicka E, Zak K, Szczygielski O. Age related changes in brain MR appearance in the course of neurocutaneous melanosis. Eur J Radiol [Internet]. 2016 Aug [citado 2017 Jan 20];85(8):[about 5 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27423683
6.Guégan S, Kadlub N, Picard A, Rouillé T, Charbel C, Coulomb-L'Hermine A, et al. Varying proliferative and clonogenic potential in NRAS-mutated congenital melanocytic nevi according to size. Exp Dermatol [Internet]. 2016 Oct [citado 2017 Jan 20];25(10):[about 5 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27193390
7.Salgado CM, Basu D, Nikiforova M, Hamilton RL, Gehris R, Jakacki R, et al. Amplification of mutated NRAS leading to congenital melanoma in neurocutaneous melanocytosis. Melanoma Res [Internet]. 2015 Oct [citado 2017 Jan 20];25(5):[about 8 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/26266759
8.Gorai S, Saha M, Seth J. Giant Congenital Melanocytic Nevus with Occipital Encephalocele: A Very Rare Association. Indian J Dermatol [Internet]. 2016 Mar-Apr [citado 2017 Jan 20];61(2):[about 3 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27057033
9.Rao AG. Bilateral Symmetrical Congenital Giant Becker's Nevus: A Rare Presentation. Indian J Dermatol [Internet]. 2015 Sep-Oct [citado 2017 Jan 20];60(5):[about 522 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/26538733
10.Captier G. The congenital melanocytic nevi of the face in child: What's new. Rev Stomatol Chir Maxillofac Chir Orale [Internet]. 2015 Sep [citado 2017 Jan 20];116(4):[about 13 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/26189003
11.Ramesh R, Shaw N, Miles EK, Richard B, Colmenero I, Moss C. Mosaic NRAS Q61R mutation in a child with giant congenital melanocytic naevus, epidermal naevus syndrome and hypophosphataemic rickets. Clin Exp Dermatol [Internet]. 2017 Jan [citado 2017 Feb 13];42(1):[about 5 p.]. Available from: http://onlinelibrary.wiley.com/doi/10.1111/ced.12969/full
12.Kinsler VA, O'Hare P, Jacques T, Hargrave D, Slater O. MEK inhibition appears to improve symptom control in primary NRAS-driven CNS melanoma in children. Br J Cancer [Internet]. 2017 Apr 11 [citado 2017 Jun 22];116(8):[about 4 p.]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/28253523
Published
How to Cite
Issue
Section
License
Copyright (c) 2017 Elayne Esther Santana Hernández, Rafael Alfredo LLauradó Robles

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright: Camagüey Medical Archive Magazine, offers immediately after being indexed in the SciELO Project; Open access to the full text of the articles under the principle of making available and free the research to promote the exchange of global knowledge and contribute to a greater extension, publication, evaluation and extensive use of the articles that can be used without purpose As long as reference is made to the primary source.
Conflicts of interest: authors must declare in a mandatory manner the presence or not of conflicts of interest in relation to the investigation presented.
(Download Statement of potential conflicts of interest)
The Revista Archivo Médico de Camagüey is under a License Creative Commons Attribution-Noncommercial-No Derivative Works 4.0 International (CC BY 4.0).
This license allows others to distribute, to mix, to adjust and to build from its work, even for commercial purposes, as long as it is recognized the authorship of the original creation. This is the most helpful license offered. Recommended for maximum dissemination and use of licensed materials. The full license can be found at: https://creativecommons.org/licenses/












 22 julio 2025
22 julio 2025