In vitro inhibitory effect of fosfomycin trometamol and cefoperazone sulbactam on Enterobacteriaceae producing ESBL
Abstract
Introduction: Urinary tract infections represent a significant challenge in public health, particularly due to the limited availability of antimicrobial agents to treat resistant microorganisms, such as extended-spectrum beta-lactamase producing enterobacteria.
Objective: To evaluate the in vitro activity of fosfomycin and cefoperazone/sulbactam against ESBL strains isolated from urinary tract infections and asymptomatic bacteriuria at the Lambayeque Regional Hospital from 2018 to 2020.
Methods: An observational descriptive study was conducted, analyzing 268 ESBL strains divided into groups based on their origin, stemming from both urinary tract infections (UTIs) and cases of asymptomatic bacteriuria. The presence of ESBL was confirmed using the Jarlier test, and identification was performed using the Vitek 2 system. Susceptibility to cefoperazone/sulbactam and fosfomycin trometamol was assessed using the Kirby-Bauer method.
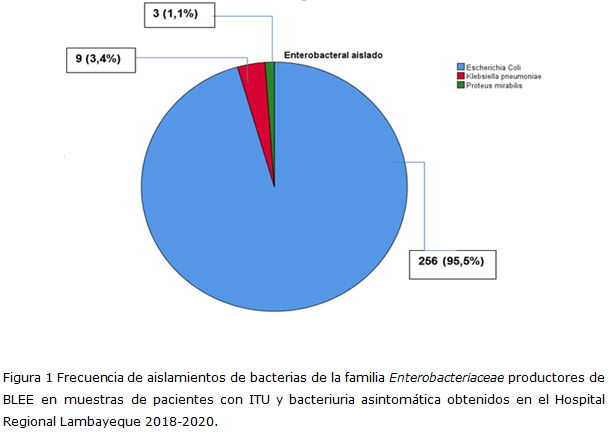
Results: 95.5% of the isolated bacteria were ESBL-producing E. coli. According to CLSI criteria, 99.3% were susceptible to fosfomycin, while under EUCAST criteria, susceptibility was 91.8%. The susceptibility to cefoperazone/sulbactam was 91.4%. The average inhibition zone diameters for fosfomycin and cefoperazone/sulbactam were 25.14 mm and 22.5 mm, respectively.
Conclusions: Both cefoperazone/sulbactam and fosfomycin demonstrated a high in vitro inhibitory effect against ESBL-producing bacteria, making them excellent candidates for future clinical studies. The observed susceptibility in asymptomatic bacteriuria cases indicates that there is no silent reservoir of resistance to these drugs that could rapidly increase with more widespread use.
DeCS: DISEASE SUSCEPTIBILITY; URINARY TRACT INFECTIONS; BETA-LACTAM RESISTANCE; BACTERIURIA; ESCHERICHIA COLI.
Downloads
References
1. Tandogdu Z, Wagenlehner FME. Global epidemiology of urinary tract infections. Curr Opin Infect Dis [Internet]. 2016 [citado 9 Sep 2024];29(1):73–9. Disponible en: https://doi.org/10.1097/qco.0000000000000228
2. Pigrau C. Infección del tracto urinario [Internet]. Barcelona: SALVAT; 2013 [citado 19 Sep 2024]. Disponible en: https://www.seimc.org/contenidos/documentoscientificos/otrosdeinteres/seimc-dc2013-LibroInfecciondeltractoUrinario.pdf
3. Givler DN, Givler A. Asymptomatic Bacteriuria [Internet]. Treasure Island: StatPearls Publishing; 2022[citado 20 Sep 2024]. Disponible en: https://pubmed.ncbi.nlm.nih.gov/28722878/
4. Santamaría-Veliz O, Aguilar-Gamboa FR, Serquén-López LM, Díaz-Maldonado KC, López-Ramírez KL, Silva-Díaz H; et al. Clonalidad de cepas de Escherichia coli productoras de β-lactamasas de espectro extendido aisladas de pacientes con infección urinaria de la comunidad y portadores asintomáticos de un hospital de Chiclayo. Revista Experiencia en Medicina [Internet]. 2019[citado 20 Sep 2024];5(3):126–34. Disponible en: https://doi.org/10.37065/rem.v5i3.368
5. Aguilar-Gamboa FR. Impacto del uso irracional de antimicrobianos durante la pandemia por COVID-19. Rev Exp en Med del Hosp Reg Lambayeque [Internet]. 2022 [citado 9 Sep 2024];8(2). Disponible en: http://www.rem.hrlamb.gob.pe/index.php/REM/article/view/368
6. Maslikowska JA, Walker SAN, Elligsen M, Mittmann N, Palmay L, Daneman N; et al. Impact of infection with extended-spectrum β-lactamase-producing Escherichia coli or Klebsiella species on outcome and hospitalization costs. J Hosp Infect [Internet]. 2016 [citado 9 sep 2024];92(1):33–41. Disponible en: https://www.journalofhospitalinfection.com/article/S0195-6701(15)00386-2/abstract
7. Corvec S, Furustrand Tafin U, Betrisey B, Borens O, Trampuz A. Activities of Fosfomycin, Tigecycline, Colistin, and Gentamicin against Extended-Spectrum-β-Lactamase-Producing Escherichia coli in a Foreign-Body Infection Model. Antimicrob Agents Chemother [Internet]. 2013 [citado 9 Sep 2024];57(3):1421–7. Disponible en: https://doi.org/10.1128/AAC.01718-12
8. Banerjee S, Sengupta M, Sarker T. Fosfomycin susceptibility among multidrug-resistant, extended-spectrum beta-lactamase-producing, carbapenem-resistant uropathogens. Indian J Urol [Internet]. 2017 [citado 9 Sep 2024];33(2):149. Disponible en: https://doi.org/10.4103/iju.iju_285_16
9. Lai CC, Chen CC, Lu YC, Lin TP, Chuang YC, Tang HJ. Appropriate composites of cefoperazone & ndash; sulbactam against multidrug-resistant organisms. Infect Drug Resist [Internet]. 2018 [citado 9 Sep 2024]; 11:1441–5. Disponible en: https://pubmed.ncbi.nlm.nih.gov/30237728/
10. Patel B, Patel K, Shetty A, Soman R, Rodrigues C. Fosfomycin Susceptibility in Urinary Tract Enterobacteriaceae. J Assoc Physicians India [Internet]. 2017 [citado 9 Sep 2024];65(9):14–6. Disponible en: http://www.ncbi.nlm.nih.gov/pubmed/29313570
11. World Health Organization. Antimicrobianos de importancia crítica para la medicina humana, 6.a revisión, 2018 [Internet]. Ginebra: Organización Mundial de la Salud; 2019 [citado 20 Sep 2024]. Disponible en: https://apps.who.int/iris/bitstream/handle/10665/331531/9789243515526spa.pdf?sequence=5&isAllowed=y
12. Williams PC. Potential of fosfomycin in treating multidrug‐resistant infections in children. J Paediatr Child Health [Internet]. 2020 [citado 9 Sep 2024];56(6):864–72. Disponible en: https://doi.org/10.1111/jpc.14883
13. Clinical and Laboratory Standards Institute (CLSI). CLSI M100-ED32:2022 Performance Standards for Antimicrobial Susceptibility Testing, 35nd Edition [Internet]. Estados Unidos: CLSI; 2022[citado 20 Jan 2025]. Disponible en: https://cdn.bfldr.com/YLD4EVFU/at/hvshwc8rxbsbnnmtqp9f3886/m100ed35e_sample.pdf
14. EUCAST [Internet]. The European Committee on Antimicrobial Susceptibility Testing; 2025 [actualizado 2025; citado 20 Oct 2024]. Clinical breakpoints - and guidance [about 2]. Disponible en: https://www.eucast.org/fileadmin/src/media/PDFs/EUCAST_files/Breakpoint_tables/v_12.0_Breakpoint_Tables.pdf
15. Hernández Sampieri R, Fernández Collado C, Baptista Lucio MP. Metodología de la Investigación [Internet]. Mexico: Mc Graw Hill; 2014 [citado 9 Sep 2024]. Disponible en:https://www.esup.edu.pe/wpcontent/uploads/2020/12/2.%20Hernandez,%20Fernandez%20y%20Baptista-metodolog%C3%ADa%20Investigacion%20Cientifica%206ta%20ed.pdf
16. Gehringer C, Regeniter A, Rentsch K, Tschudin-Sutter S, Bassetti S, Egli A. Accuracy of urine flow cytometry and urine test strip in predicting relevant bacteriuria in different patient populations. BMC Infect Dis [Internet]. 2021 [citado 9 Sep 2024];21(1):209. Available from: https://doi.org/10.1186/s12879-021-05893-3%0A%0A
17. Sacsaquispe Contreras R, Velásquez Pomar J. Manual de procedimientos para la prueba de sensibilidad antimicrobiana por el método de disco difusión [Internet]. Lima: Instituto Nacional de salud; 2002[citado 20 Sep 2024]. Disponible en: https://antimicrobianos.ins.gob.pe/images/contenido/documentos/nacionales/manua_l_sensibilidad.pdf
18. Naushad VA, Purayil NK, Wilson GJ, Chandra P, Joseph P, Khalil Z; et al. Epidemiology of urinary tract infection in adults caused by extended-spectrum beta-lactamase (ESBL)-producing Enterobacteriaceae – a case–control study from Qatar. IJID Reg [Internet]. 2022 [citado 9 Sep 2024]; 3:278–86. Disponible en: https://doi.org/10.1016/j.ijregi.2022.05.001
19. Najafi A, Hasanpour M, Askary A, Aziemzadeh M, Hashemi N. Distribution of pathogenicity island markers and virulence factors in new phylogenetic groups of uropathogenic Escherichia coli isolates. Folia Microbiol (Praha) [Internet]. 2018 [citado 9 Sep 2024];63(3):335–43. Disponible en: https://doi.org/10.1007/s12223-017-0570-3
20. Matta-Chuquisapon J, Valencia-Bazalar E, Marocho-Chahuayo L, Gonzales-Escalante E, Sevilla-Andrade CR. Presencia de genes fimH y afa en aislamientos urinarios de Escherichia coli productora de betalactamasas de espectro extendido en Lima, Perú. Rev Peru Med Exp Salud Publica [Internet]. 2020 [citado 9 Sep 2024];37(2):282–6. Disponible en: http://dx.doi.org/10.17843/rpmesp.2020.372.4829 %0
21. Stahlhut SG, Tchesnokova V, Struve C, Weissman SJ, Chattopadhyay S, Yakovenko O; et al. Comparative Structure-Function Analysis of Mannose-Specific FimH Adhesins from Klebsiella pneumoniae and Escherichia coli. J Bacteriol [Internet]. 2009 [citado 9 sep 2024];191(21):6592–601. Disponible en: https://doi.org/10.1128%2FJB.00786-09
22. Habibi M, Asadi Karam MR, Bouzari S. In silico design of fusion protein of FimH from uropathogenic Escherichia coli and MrpH from Proteus mirabilis against urinary tract infections. Adv Biomed Res [Internet]. 2015 [citado 20 Sep 2024]; 4:217. Disponible en: https://pubmed.ncbi.nlm.nih.gov/26605246/
23. Aguilar-Martínez SL, Suclupe-Campos DO, Guevara-Vásquez GM, Failoc-Rojas VE, Aguilar-Gamboa FR. Factores asociados a la colonización rectal por Enterobacteriaceae productoras de betalactamasas de espectro extendido en pacientes de consulta externa de un hospital al norte del Perú. Rev del Cuerpo Médico Hosp Nac Almanzor Aguinaga Asenjo [Internet]. 2022 [citado 9 Sep 2024];15(1):46–52. Disponible en: https://doi.org/10.35434/rcmhnaaa.2022.151.965
24. Taylor C, Abbey BS, Eszter D. What’s New from the CLSI Subcommittee on Antimicrobial Susceptibility Testing M100,29th Edition [Internet]. 2019 [ciatdo 9 Sep 2024]. Disponible en:
https://clsi.org/media/3062/clsi-update2019_21819_final_fullsizedhandouts.pdf
25. Aguilar-Gamboa FR, Aguilar Martinez SL, Cubas Alarcón DM, Coaguila Cusicanqui LÁ, Fernández Valverde DA, Mario Cecilio MM; et al. Portadores de bacterias multirresistentes de importancia clínica en áreas críticas (UCI-UCIN) de un hospital al norte del Perú. Horiz Médico [Internet]. 2016 [citado 9 Sep 2024];16(3):50–7. Disponible en: https://www.horizontemedico.usmp.edu.pe/index.php/horizontemed/article/view/470
26. Mothibi LM, Bosman NN, Nana T. Fosfomycin susceptibility of uropathogens at Charlotte Maxeke Johannesburg Academic Hospital. South African J Infect Dis [Internet]. 2020 [citado 9 Sep 2024];35(1). Disponible en: https://doi.org/10.4102%2Fsajid.v35i1.173
27. Lima RC, Faria CA, Carraro-Eduardo JC, Morales PS, Fonseca ABM. Evaluation of sensitivity profiles to fosfomycin in bacterial urine samples from outpatients. Eur J Obstet Gynecol Reprod Biol [Internet]. 2021 [citado 9 Sep 2024]]; 262:1847. Disponible en: https://pubmed.ncbi.nlm.nih.gov/34034198/
28. Hussain T, Moqadasi M, Malik S, Salman Zahid A, Nazary K, Khosa SM; et al. Uropathogens Antimicrobial Sensitivity and Resistance Pattern From Outpatients in Balochistan, Pakistan. Cureus [Internet]. 2021 [citado 17 Sep 2024]: 13(8):e17527. Disponible en: https://pubmed.ncbi.nlm.nih.gov/34646592/
29. Hussain-Gilani SY, Ali Shah SR, Ahmad N, Bibi S. Antimicrobial Resistance Patterns In Community Acquired Urinary Tract Infections. J Ayub Med Coll Abbottabad [Internet]. 2016 [citado 9 Sep 2024];28(3):572–4. Disponible en: http://www.ncbi.nlm.nih.gov/pubmed/28712238
30. Varela EA. Rotación de antibióticos: una estrategia para paliar la resistencia. Rev CENIC Ciencias Biológicas [Internet]. 2006 [citado 9 Sep 2024];37(1):37–44. Disponible en: https://www.redalyc.org/pdf/1812/181220542007.pdf
31. Cusack TP, Ashley EA, Ling CL, Rattanavong S, Roberts T, Turner P; et al. Impact of CLSI and EUCAST breakpoint discrepancies on reporting of antimicrobial susceptibility and AMR surveillance. Clin Microbiol Infect [Internet]. 2019 [citado 9 sep 2024];25(7):910–1. Disponible en: https://doi.org/10.1016%2Fj.cmi.2019.03.007
32. Gardiner BJ, Stewardson AJ, Abbott IJ, Peleg AY. Nitrofurantoin and fosfomycin for resistant urinary tract infections: old drugs for emerging problems. Aust Prescr [Internet]. 2019 [citado 9 Sep 2024];42(1):14. Disponible en: https://doi.org/10.18773/austprescr.2019.002
33. Sardar A. Comparative Evaluation of Fosfomycin Activity with other Antimicrobial Agents against E.coli Isolates from Urinary Tract Infections. J Clin DIAGNOSTIC Res [Internet]. 2017 [citado 9 Sep 2024]; Disponible en: https://jcdr.net/articles/PDF/9440/23644_CE[Ra1]_F(RK)_PF1(PI_RK)_PFA(AK)_PF2(P_RK)_PF3(AG_OM).pdf
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Franklin Rómulo Aguilar-Gamboa, Martha Arminda Vergara-Espinoza

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Copyright: Camagüey Medical Archive Magazine, offers immediately after being indexed in the SciELO Project; Open access to the full text of the articles under the principle of making available and free the research to promote the exchange of global knowledge and contribute to a greater extension, publication, evaluation and extensive use of the articles that can be used without purpose As long as reference is made to the primary source.
Conflicts of interest: authors must declare in a mandatory manner the presence or not of conflicts of interest in relation to the investigation presented.
(Download Statement of potential conflicts of interest)
The Revista Archivo Médico de Camagüey is under a License Creative Commons Attribution-Noncommercial-No Derivative Works 4.0 International (CC BY 4.0).
This license allows others to distribute, to mix, to adjust and to build from its work, even for commercial purposes, as long as it is recognized the authorship of the original creation. This is the most helpful license offered. Recommended for maximum dissemination and use of licensed materials. The full license can be found at: https://creativecommons.org/licenses/












 22 julio 2025
22 julio 2025